Hormones. Can’t live with them, can’t live (comfortably) without them. Right?
If you are like most women who have low levels of progesterone, you probably feel like you’ve completely lost control of your body!
And the worst part of it all…
Is anyone taking the time to actually listen to you and put together the pieces of this hormonal puzzle? A puzzle filled with pieces that either don’t fit, are missing, or have changed.
Is your voice being heard?
The voice that is screaming in frustration with crazy PMS (think anxiety, bad moods, sore boobs and bloating), heavy periods and spotting…not a happy place or a good look!
What is progesterone and why is it important?
Progesterone is a powerhouse steroid hormone that is necessary for healthy menstrual cycles and overall health.
Progesterone (when in balance with estrogen) supports:
- Brain health and cognitive function1,3,4
- Nervous system support
- Improved sleep quality5
- Bone health/density 1,6
- Skin health – too much estrogen in relation to progesterone can cause melasma (brown spots on the face. Estrogen increases pigmentation and progesterone reduces it.
- The lining of the uterus (endometrium) to allow a fertilized egg to make a rather cozy home for a fetus1
- Prevention of miscarriage and early labor1
In case you’re wondering, progesterone is produced in a few places in the body:1
- The adrenal glands
- The corpus luteum that forms on the ovary after ovulation; the corpus luteum produces progesterone during early pregnancy as well
- In the placenta during later pregnancy
Ovulation – how we make most of our progesterone
If I had a dollar for every time someone has asked me how they can make more progesterone I’d legit be able to retire tomorrow! This is the age-old question, and my answer is always the same…
“Do you ovulate? If so, do you ovulate regularly?”
Meaning, you have a period every 25-35 days consistently and you are confirming ovulation through basal body temperature rises and/or cervical fluid changes.
If you answer NO or I DON’T KNOW to this question, then I refer you to chapter 1 of my book where I explain how to track basal temperature and cervical fluid to determine if/when you are ovulating.
ICYMI: Thanks to progesterone’s heat-inducing qualities, it actually raises your body temperature. This rise in temperature gives you the heads up that you’ve likely ovulated!7 This is so important when tracking your period. Find out which period tracking apps I like the best here!
If you answer YES to this question, and you still experience symptoms associated with progesterone deficiency, then I refer you to the 6-week protocol in my book starting at chapter 4. This protocol will support your sweet little ovaries to have a healthy-as-can-be ovulation, and ultimately adequate progesterone production.
Let me reiterate. Ovulation that happens regularly is the only way to make enough progesterone for you to feel good. I’ll get to how to have healthy ovulations in a bit!
The difference between low progesterone, estrogen dominance and excess estrogen
The next question I get ALL the time goes something like this:
“What is estrogen dominance? And is there a difference between low progesterone and estrogen dominance/excess estrogen?”
Simply put, estrogen dominance means that estrogen is too high in relation to progesterone. That is it! It’s not complicated. These two sister hormones have to play nice with each other in order for you to feel good and not have period & mood problems.
You can be estrogen dominant and have low estrogen. Seems weird, I know. But if your estrogen is too high in relation to your progesterone (even if it is low), you are technically estrogen dominant.
Excess estrogen is just another way of saying estrogen dominant. It means you have too high estrogen in relation to progesterone.
There are five scenarios I see in my practice to help explain this better:
- High estrogen, normal progesterone
- High estrogen, low progesterone
- Normal estrogen, low progesterone
- Low estrogen, even lower progesterone
- Normal estrogen, normal progesterone but the person is exposed to too many xenoestrogens (usually through environmental chemicals that are estrogen mimickers in the body), which creates symptoms of estrogen dominance.
All of these scenarios equal estrogen dominance and will likely produce the same symptoms. Don’t forget, progesterone has a system-wide effect on the body (brain, bones, sleep and periods), which is why you feel so many symptoms that seem almost unrelated.
- Gnarly PMS – mood swings, anxiety, overwhelm, feeling like you can’t cope, aching, pain, crampiness, migraines and headaches,12,13 water retention, bloating and painful breasts
- Spotting 3 or more days before your period begins
- Thickened uterine lining which can lead to heavy (more than 80ml per period) and/or long periods (those lasting more than 8 days), and clotty periods that don’t flow well
- Shortened luteal phase (less than 10 days long)
- Acne and/or melasma
- Period pain – progesterone is a feel-good, anti-inflammatory hormone that reduces pain
- Insomnia or difficulty sleeping in the luteal phase
- Gallbladder problems (too much estrogen isn’t good for the gallbladder)
- Worsening of conditions that are impacted by estrogen like uterine fibroids, ovarian cysts, endometriosis and adenomyosis
Longterm, the lining of the uterus can become too thick which is a risk factor for uterine cancer.1,2
For all my pregnant folks – when progesterone is low during pregnancy you may experience symptoms like:12
- Miscarriage
- Vaginal spotting
- Abdominal pain
- Low blood sugar
- Breast tenderness
- Fatigue
- Vaginal dryness

What causes low progesterone?
Brace yourself kids, this is a long list.
But remember a very important point – ALL of these things do one major thing – repeat after me – they disrupt ovulation.
They either delay it (and it becomes sporadic or irregular), stop it completely (anovulation) or affect the health of the corpus luteum thus affecting the amount of progesterone it releases. So, here goes…
- Ongoing or excess psychological stress (when in fight or flight, the body feels like it’s in too much danger to ovulate)10,11
- Inflammation in the body and brain inflammation (this will impact brain signaling to the ovaries)
- Thyroid problems or thyroid disease
- PCOS, diabetes (mismanaged) and blood sugar problems
- Gut health problems and subsequent poor absorption of nutrients
- Obesity which leads to the release of too much estrogen tricking the body into thinking it is on hormonal birth control8
- Over-exercise or over-training
- Being underweight which causes the body to stop producing estrogen leading to irregular cycles, missing cycles, and lack of ovulation8
- Perimenopause
- Hyperprolactinemia (high levels of prolactin suppress ovulation)
- Excess melatonin (in the form of supplementation)
- Hysterectomy
- Low cholesterol (not enough raw material to make steroid hormones)
- Problems with your mitochondria (your ovaries are mitochondria powerhouses)
- Ongoing infections (chronic Lyme or Epstein Barr, dental infections
- Progestin-based IUD’s (Mirena, Skyla, Kyleena etc) I know you may have been told you’ll still ovulate but that’s just not true for everyone
- Blood flow stagnation in the pelvic region (reduces blood flow to the reproductive organs)
I know this seems like a long ass list, but it’s so important to remember that there are solutions for every one of these problems. And for the most part, they are all the same. Hang tight for those.
And once you start to check each off the list, you’ll see improvements in your ovarian function and progesterone levels.
How to know if you are ovulating
As I said before, the first step in figuring out if/when you are ovulating is to have a better understanding of your cycle so check out my post, The Four Phases of Your Menstrual Cycle. Understanding how your hormones work in each phase of your cycle is key to understanding when you may ovulate each month.
Finding a way to track your menstrual cycle is needed to determine if/when you are ovulating so, finding a reliable tracking method is key and yes, there’s an app for that!
So, you have a period tracker…now what?
Most importantly, you are going to need a good basal thermometer (it measures basal body temperature) to see when things start to heat up! I have a few fav’s that are my go-to which you can check out here.
Your basal temperature rises 2/10th’s of a degree or higher a few days post ovulation, which is your sign that ovulation has occurred. This is what you want to be looking out for when tracking your temperature.
I explain exactly how to do all of this on pages 26-30 in my book Fix Your Period.
If you’re more interested in using this method for birth control, check out my article on the Fertility Awareness Method which involves checking your basal body temperature and cervical fluid each day. It’s not as hard as it sounds, I promise!
When and how to test hormones to check progesterone levels
No one has a cookie-cutter menstrual cycle, so knowing when to test your progesterone levels can be tricky. You may have heard that the best time to test progesterone is on day 21 of your cycle. This is based on ovulation happening on day 14 of your cycle and then testing 7 days after ovulation.
But this time frame won’t work for everyone! Progesterone only rises after you’ve already ovulated, which means that if you test too early (pre-ovulation), the results will not be an accurate representation of what’s happening with your hormones.
So here’s the question. “When exactly should I test my progesterone?”
Well, first you need to go back to your period tracker of choice and check your temperature fluctuations (and cervical fluid patterns if you’re tracking those) to determine when you had the “Big O”. Progesterone should be tested 5-7 days after ovulation day. If you ovulated on day 16, you’d want to test on days 21, 22, or 23.
If you don’t know when you ovulated, and you have a regular period (it comes every 25-35 days consistently), check your period tracker and count back 7 days to when your period is due. If your period is irregular, I highly recommend you track your temperature to get a more accurate idea of when you ovulated so you test on the right day.
What to do if your progesterone levels are low?
See my article on when to test progesterone for ideal progesterone numbers.
As I mentioned before, less than optimal progesterone levels are 100% linked to either lack of ovulation or irregular ovulation. So really, it is just a symptom of the multiple causes I described above.
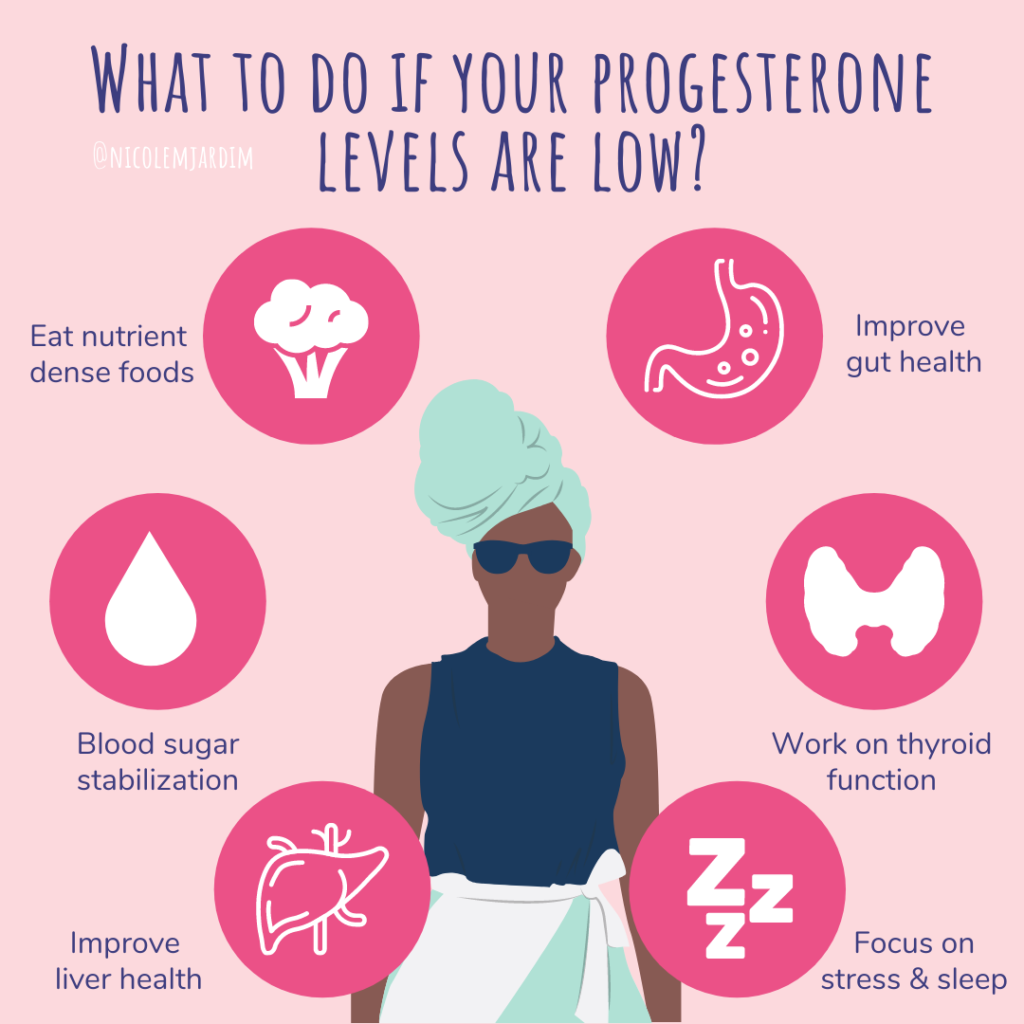
In my book Fix Your Period I outline 6 pillars to consistent ovulation and optimal progesterone production.
- Nutrient dense foods with a focus on leafy green veggies, cruciferous veggies, complex carbs and high quality protein and fat. This includes eating enough so your body doesn’t feel like it’s in starvation mode.
- Blood sugar stabilization – if there was anything I recommended ever, this would be it. Dysregulated blood sugar directly negatively affects the ovaries!
- Gut health – the health of your gut will have a systemwide effect. It even determines estrogen levels because it plays a role in the breakdown and excretion of estrogen.
- Liver health – your liver breaks down toxins and hormones via two pathways. If those pathways don’t have the raw materials to work properly, you’ll run into problems.
- Stress and sleep – stress will literally stop ovulation if you let it get out of control. Lack of sleep is a stressor that your ovaries don’t take kindly to either.
- Thyroid function – your thyroid gland and your ovaries are like close cousins. They work in tandem with each other to support ovulation and progesterone production.
So where to start? Make it easy. Choose one of these 6 pillars – the one that is either easiest for you or the one you know you need to work on the most – and work on it. Then move onto the next one.
There is no magic bullet, no other way to fix your progesterone problems than to support your foundation. Can’t build a big beautiful house on sticks. Building the concrete foundation isn’t so exciting, but eventually you have a house and you get to do the fun decorating.
Take my period quiz to start learning why this is happening to you and the best next steps for your body!
Then grab my book Fix Your Period and my Harness Your Hormones 28-Day Reset Program bundle.
References:
1. Cable JK, Grider MH. Physiology, Progesterone. [Updated 2020 Jun 4]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK558960/
2. Kim, J. J., & Chapman-Davis, E. (2010). Role of progesterone in endometrial cancer. Seminars in reproductive medicine, 28(1), 81–90. https://doi.org/10.1055/s-0029-1242998
3. Zárate, S., Stevnsner, T., & Gredilla, R. (2017). Role of Estrogen and Other Sex Hormones in Brain Aging. Neuroprotection and DNA Repair. Frontiers in aging neuroscience, 9, 430. https://doi.org/10.3389/fnagi.2017.00430
4. Cutter, W.J., Norbury, R., & Murphy, DGM. (2003, July 1). Oestrogen, brain function, and neuropsychiatric disorders. J Neurol Neurosurg Psychiatry. https://jnnp.bmj.com/content/jnnp/74/7/837.full.pdf
5. Andersen ML, Bittencourt LR, Antunes IB, Tufik S. Effects of progesterone on sleep: a possible pharmacological treatment for sleep-breathing disorders? Curr Med Chem. 2006;13(29):3575-82. doi: 10.2174/092986706779026200. PMID: 17168724.
6. Prior JC. Progesterone for the prevention and treatment of osteoporosis in women. Climacteric. 2018 Aug;21(4):366-374. doi: 10.1080/13697137.2018.1467400. Epub 2018 Jul 2. PMID: 29962257.
7. Su, H. W., Yi, Y. C., Wei, T. Y., Chang, T. C., & Cheng, C. M. (2017). Detection of ovulation, a review of currently available methods. Bioengineering & translational medicine, 2(3), 238–246. https://doi.org/10.1002/btm2.10058
8. Weight, Fertility, and Pregnancy. (2018). Retrieved on March 17, 2021 from https://www.womenshealth.gov/healthy-weight/weight-fertility-and-pregnancy
9. Gude D. (2011). Thyroid and its indispensability in fertility. Journal of human reproductive sciences, 4(1), 59–60. https://doi.org/10.4103/0974-1208.82368
10. Whirledge S, Cidlowski JA. Glucocorticoids, stress, and fertility. Minerva Endocrinol. 2010 Jun;35(2):109-25. PMID: 20595939; PMCID: PMC3547681.
11. Toufexis, D., Rivarola, M. A., Lara, H., & Viau, V. (2014). Stress and the reproductive axis. Journal of neuroendocrinology, 26(9), 573–586. https://doi.org/10.1111/jne.12179
12. Feintuch, S. (2017, March 17) .Retrieved on February 27, 2021 from https://www.healthywomen.org/your-health/low-progesterone-symptoms
13. Fish, S. (2019, October). Retrieved on February 27, 2021 from https://www.hormone.org/your-health-and-hormones/glands-and-hormones-a-to-z/hormones/progesterone




4 thoughts on “Low Progesterone: Why it happens and what you can do about it”
What you think about Vitex? I’m using for a month and my spoot dropped from 10 to 4 days
It can be helpful for some people but it isn’t for everyone. Additionally, as I said multiple times above, it can’t fix underlying nutrient deficiencies etc. So it could be a good addition to everything else. I wrote a detailed article about vitex for further reading. You can search for it in the search bar.
Hello,
Which source did you find low cholesterol as a cause of low progesterone? My doctor said that could not be a reason, but I would like to read the research myself. I am finding research about high cholesterol, but not low.
Hi there! Your doctor is either willfully ignorant or missed the lesson in medical school on how steroid hormones are made?
The first step in steroid hormone synthesis involves the STAR protein, which comes from the STAR gene. STAR stands for steroidogenic acute regulatory protein. The STAR protein binds to cholesterol in the mitochondria of the adrenal glands, gonads and other glands and organs to form pregnenolone, the “mother hormone.” Pregnenolone leaves the mitochondria and is then converted to various steroid hormones in specific glands, organs and tissues.
Dietary fat supports so many aspects of our menstrual cycle health and fertility, due to the fact that our livers and intestines use healthy fats to make cholesterol, a building block for some of our most important steroid hormones, such as progesterone, estrogen, and testosterone.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4707056/